An acoustic neuroma – or a vestibular Schwannoma – is a non-cancerous brain tumour or growth, which develops on the nerve connecting the ear to the brain. This facial nerve carries information from the brain to the face muscles.
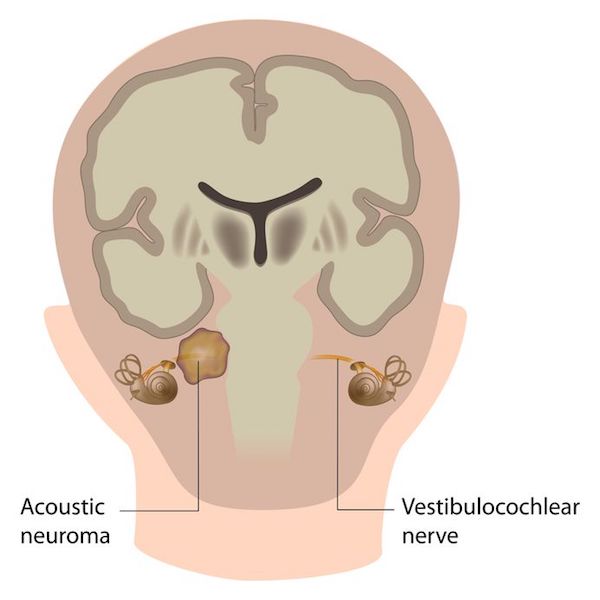
Acoustic neuromas grow from the cells that cover the vestibulocochlear nerve, called Schwann cells. If the tumour grows large enough, it can press against the brain cause hearing loss, ringing in the ear and unsteadiness, and may become life threatening.
Acoustic neuroma causes are unknown, but a small percentage of cases (about 5%) are caused by a rare, genetic condition called neurofibromatosis type 2.
Age is a factor in prevalence, with most acoustic neuromas reportedly diagnosed in patients aged between 30 and 60. They are more common in women than men.
What are its symptoms?
Symptoms may develop gradually because acoustic neuromas grow slowly. In the case of a small acoustic neuroma, there may not be any symptoms at all.
Acoustic neuromas typically grow about 1 to 2mm every year; however, there are periods when it stops growing.
Acoustic neuroma symptoms may include:
- Ataxia (loss of physical co-ordination)
- Balance problems
- Ear pain
- Loss of taste
- Memory loss
- Hearing loss (usually develops gradually in one ear)
- Tinnitus (the perception of noise in one or both ears)
- Vertigo (the feeling that you or the environment around you is spinning)
- Facial paralysis
- Facial tingling or pain
- Headaches: Although rare, this may occur if the tumour blocks the flow of cerebrospinal fluid around your brain
- Temporary vision problems: Caused by cerebrospinal fluid blockage but also rare
How is it diagnosed?
An acoustic neuroma diagnosis can be difficult as the symptoms are similar to those of middle-ear problems. Symptoms, such as dizziness and hearing loss, are also similar to other conditions, such as Ménière’s disease (a rare disorder affecting the inner ear).
If your doctor suspects you have acoustic neuroma, he/she will refer you to a hospital or clinic for further testing.
The three types of diagnostic tests for acoustic neuroma are:
- Hearing tests: You may undergo one of a number of hearing tests including a pure tone audiometry test and a speech recognition audiometry test.
- Magnetic resonance imaging (MRI) scan: This allows your doctor to see the size and position of your tumour, and is considered one of the most accurate forms of diagnosis.
- Computerised tomography (CT) scan: X-rays and a computer are used to create detailed internal images of the body, including internal organs, blood vessels, bones and tumours.
What are your treatment options?
Acoustic neuroma treatment may vary, depending on the size of the tumour and symptoms. Treatments include monitoring, radiation and surgery.
To monitor the tumour’s growth, your doctor may recommend that you have regular imaging and hearing tests, usually every six to 12 months. If there are further symptoms or other difficulties, you may need to undergo treatment.
This includes:
- Stereotactic radiosurgery: This aims to stop the tumour’s growth, and preserve the facial nerve’s function as well as hearing. There are some risks however, which your doctor willl discuss with you.
- Surgery: Involves the removal of the acoustic neuroma. Surgery can create adverse side effects, including worsening of symptoms. These risks are often based on the size of the tumour and the surgical approach used. Your doctor will discuss these with you.
- Radiation is an alternative treatment. It doesn’t remove the tumor, but may stop it from growing or cause it to shrink.
Can it be prevented?
There is no known prevention for acoustic neuromas. They are benign, however, and do not spread to other parts of the body. Timely diagnosis and treatment can minimise their effects.
IMAGE CREDIT: 123rf.com
