Colorectal cancer is also known as colon cancer, rectal cancer or bowel cancer. It’s one of the most common cancers that affects adults worldwide – nearly 1.4 million new cases were diagnosed in 2012 and it’s the fourth most common cause of cancer death, accounting for over 600 000 deaths a year, reports Medicalnewstoday.com. Ninety percent of colorectal cancers occur in people aged 50 and older.
Little is known about the causes of colorectal cancer, also known as cancer of the large bowel. But studies have shown that its frequency is greater in countries that eat a diet high in fat and low in fibre.
Most cases of this cancer begin as small, benign clumps of cells called adenomatous polyps. Over time, some of these polyps become colon cancers. Polyps may be small and produce few, if any, symptoms. For this reason, doctors recommend regular screening tests, which help identify polyps before they become colon cancer.
Other risk factors include:
- High alcohol intake, particularly of beer
- A history of severe ulcerative colitis or Crohn’s disease, which affects the large bowel.
What are its symptoms?
The most common symptom of colorectal cancer is a change in bowel habits.
This includes:
- Diarrhoea
- Constipation
- Change in consistency of your stool
- Rectal bleeding or blood in your stool
- Abdominal discomfort
- A feeling that your bowel is not emptying completely
- Weakness or fatigue
- Weight loss.
There are often no symptoms in the early stages of the disease. When they do appear, they will vary, depending on size and location of the cancer in your large intestine.
If your symptoms have lasted six or more weeks, you need to see a specialist.
How is it diagnosed?
There are a series of tests and physical examinations to confirm or rule out a cancer diagnosis, including a digital rectal examination.
Your bowel will need to be prepared before your appointment as it must be as empty as possible so your doctor can get a clear view inside. This includes eating a high-fibre diet for a day or so before the test to clear your bowel of any residue, drinking clear fluids only the day before the exam, taking laxatives or an enema.
Test types include:
- Sigmoidoscopy or colonoscopy: The doctor passes a scope (a tube with a small camera on the end) into your bowel. A sigmoidoscopy looks at the lower part of your large bowel, while the colonoscopy looks further up the colon.
- Barium enema: This is an X-ray exam using barium, which brightens the X-ray picture. The barium is given as an enema and will outline the lower part of your bowel.
- Other tests include a blood test, abdominal ultrasound, CT scan or MRI scan.
The information from these tests is used to assess the size of the cancer and how far it has spread.
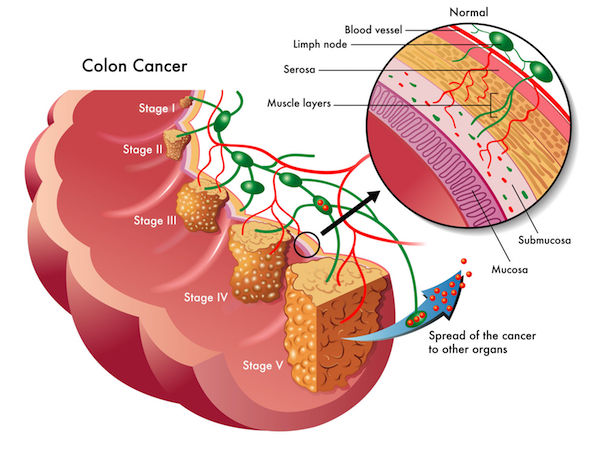
Colorectal cancer stages range from I to IV, becoming more severe and invasive as it progresses. By stage IV, the cancer has spread to distant sites, such as other organs such as your liver or lung.
What are your treatment options?
Colorectal cancer treatment will involve a multidisciplinary healthcare team, which will guide you through your cancer treatment and outline your options. Ask questions and think about all your options before deciding on your treatment.
Cancer treatments depend on the type and how advanced the cancer is, as well as your overall health and treatment preferences.
The main types of treatment for colorectal cancer are:
- Surgery: If your cancer is small, localised in a polyp and in a very early stage, your doctor may be able to remove it completely during a colonoscopy. If it is more severe, options include a partial colectomy to remove the part of your colon that contains the cancer.
- Chemotherapy: The use of drugs to kill cancer cells.
- Radiation therapy: Radiation therapy uses high-energy beams aimed at your cancer to destroy the cancer cells.
- Targeted drug therapy: Newer cancer treatments that work by targeting specific abnormalities in cancer cells.
Can it be prevented?
A key factor in colorectal cancer prevention starts with regular screening as it usually takes about 10 to 15 years for polyps to develop into colorectal cancer. Most polyps can be found and removed before they have the chance to turn into cancer. Screening can also result in finding colorectal cancer early, when it is highly curable.
People with an average risk of colon cancer should consider starting screening at age 50. But people with an increased risk, such as those with a family history of colon cancer, should consider screening sooner.
You can reduce your risk of colon cancer by making lifestyle changes. These include:
- Don't smoke
- Limit the amount of alcohol you consume
- Eat plenty of fruit and vegetables
- Exercise regularly
- Maintain a healthy weight
For more info
Cancer Association of South Africa
IMAGE CREDIT: 123rf.com
