Diabetic neuropathy is a nerve disorder that may occur in those with diabetes mellitus.
Diabetes mellitus – more commonly known as diabetes – is a condition associated with high blood sugar levels and, when poorly managed, prolonged high blood sugar levels can damage the body’s nerves. This is the cause of diabetic neuropathy.
Complications of this nerve damage can be serious: numbness of a limb may mean that sufferers are unaware of wounds and infections. Diabetic neuropathy can also lead to joint disease and urinary retention, resulting in infection.
There are four types of diabetic neuropathy:
- Peripheral (damaging the peripheral nerves, common in the legs and feet)
- Proximal (occurring in the thighs, hips or buttocks)
- Autonomic (affecting the autonomic nervous system)
- Focal (affecting a specific nerve)
What are its symptoms?
Diabetic neuropathy symptoms vary depending on the type:
- Peripheral symptoms affect the limbs and include numbness, tingling or burning, reduced ability to feel temperature changes, pain and sensitivity to touch, muscle weakness, ulcers and infections.
- Proximal neuropathy can cause pain in the hip, thigh or buttocks, usually on one side, as well as weakening of the muscles.
- Autonomic neuropathy, depending on the area affected, results in digestive and urinary symptoms, low blood pressure and dizziness if blood vessels are involved, and sexual dysfunction.
- Focal neuropathy can appear suddenly and often affects nerves in the head, legs or torso. Symptoms can include severe pain, double vision and muscle weakness.
How is it diagnosed?
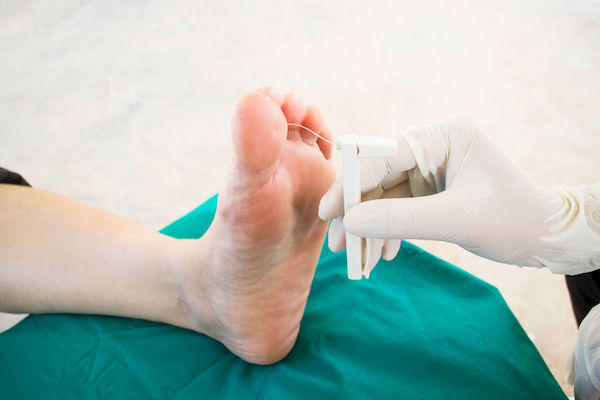
A diabetic neuropathy diagnosis is usually reached through clinical examination of a patient with diagnosed diabetes. The physical exam will include tests to check muscle strength and tone, as well as to assess reflexes and sensitivity to touch and temperature.
In cases of suspected diabetic neuropathy, nerve conduction studies to test the speed at which nerves conduct electrical impulses may be performed, often in conjunction with electromyography to measure the muscles’ electrical discharge.
It’s estimated that 45 to 55 percent of diabetes sufferers will eventually be treated for some type of associated neuropathy.
What are your treatment options?
There is no cure for this condition. Diabetic neuropathy treatment is centred around managing the symptoms, including pain relief which can rely on anti-convulsive or antidepressant medication to disrupt the neurochemical processes in the brain involved with pain perception.
Other treatments will depend on the specific complications involved, such as dietary changes for those with digestive issues, or medication to help restore sexual function or manage low blood pressure.
Treatment for diabetic neuropathy also looks at slowing its progression through careful diabetes management and adopting a healthy lifestyle with a well-balanced diet, regular physical activity and no smoking.
Can it be prevented?
Key to the prevention of diabetic neuropathy is ensuring that blood sugar levels are well managed in those with diabetes and kept within the target range at all times. Diabetics should carefully monitor their blood sugar levels and speak to their doctors if they are inconsistent, as their insulin or medication may need adjusting.
Additionally, as diabetic neuropathy often affects the legs and feet, an annual foot exam is recommended for all diabetics and it’s important to seek medical help for any persistent foot problems such as slow healing wounds, swelling or cracked skin.
What to do now
- Clicks Clinics will help you prevent, identify and manage diabetes with their wide range of screening tests and health assessments. To make an appointment at a Clicks Clinic, call 0860 254 257 or visit Clicks Clinics online and the Clicks Diabetes Management Programme.
- Visit Diabetes South Africa’s website or call 011 792-9888/7
- Visit Centre for Diabetes and Endocrinology or call 011 712 6000
IMAGE CREDIT: 123rf.com
