Glandular fever is a common and widespread type of viral infection caused by the Epstein-Barr virus.
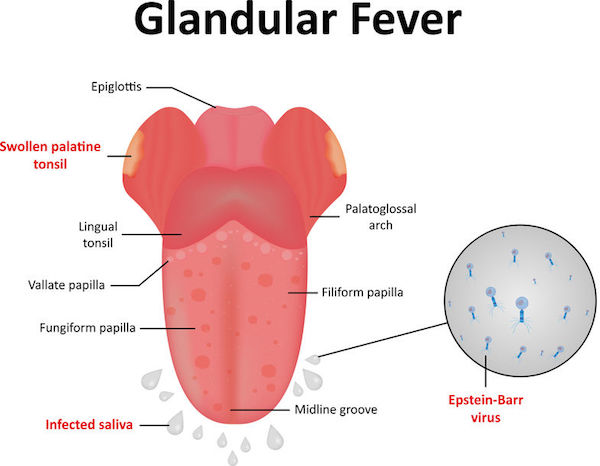
Glandular fever – also known as infectious mononucleosis (or ‘mono’), and nicknamed the ‘kissing disease’ – is a highly infectious disease that is spread via the saliva, hence the nickname.
Brought on by infection with the Epstein-Barr virus, a member of the herpes family of viruses, glandular fever causes flu-like symptoms after an incubation period of four to six weeks, or sometimes less in children.
The condition occurs most frequently in adolescents and young adults and it’s estimated that by age 40 up to 90 percent of adults have acquired immunity. Glandular fever can have serious complications should the spleen rupture or in those who are immunosuppressed.
What are its symptoms?
Glandular fever symptoms include:
- Fever, usually ranging from about 38 to 40 degrees Celsius
- Extremely sore throat. In some cases white patches may be visible on the tonsils
- Swollen lymph nodes, most notably in the neck
- Fatigue
- General feeling of being unwell
- Enlargement of the spleen
- Headache
- Body aches
- Rash on the body in a small minority of cases
- Liver enlargement and jaundice may appear in older adults, who tend to develop a more serious illness.
Symptoms of the disease can persist for up to two months or longer – while the sore throat and fever usually resolve in two to three weeks, feelings of malaise may last well beyond that.
How is it diagnosed?
If you appear to be exhibiting classic signs such as pharyngitis (sore throat), raised body temperature and enlarged lymph nodes, your healthcare provider may confirm a glandular fever diagnosis with a blood test.
Increased lymphocyte (white blood cell) levels or abnormal lymphocytes can indicate glandular fever, or the blood may be tested for the presence of antibodies to the glandular fever’s causative Epstein-Barr virus. Blood tests can also help your healthcare provider rule out other conditions that may have similar symptoms.
What are your treatment options?
As it is a self-limiting disease, glandular fever treatment options often don’t extend beyond basic self-care until symptoms have abated.
Antibiotics can’t be used to treat glandular fever since it is a viral infection, but they may be prescribed in the case of secondary infections such as tonsillitis. Medications can be used to treat fever and pain, if necessary.
It is also recommended that anyone who has had glandular fever avoid heavy exertion in the three to four weeks after the illness, to decrease the risk of the still-enlarged spleen rupturing.
Can it be prevented?
Avoiding exposure to the Epstein-Barr virus is central to the prevention of glandular fever. As it is spread through saliva, it is important not to kiss or share eating utensils with anyone who has recently been infected with the virus.
Even after recovery, the Epstein-Barr virus continues to live dormantly in the body and it can be reactivated. When this occurs the person may once again become infectious, even though they’ll often exhibit no symptoms, so avoiding the Epstein-Barr virus is not always possible as we may not even be aware of our exposure to it.
IMAGE CREDIT: 123rf.com
