A progressive bone disease characterised by loss of bone density, osteoporosis causes bones to become thin and brittle, thus increasing the risk of fractures.
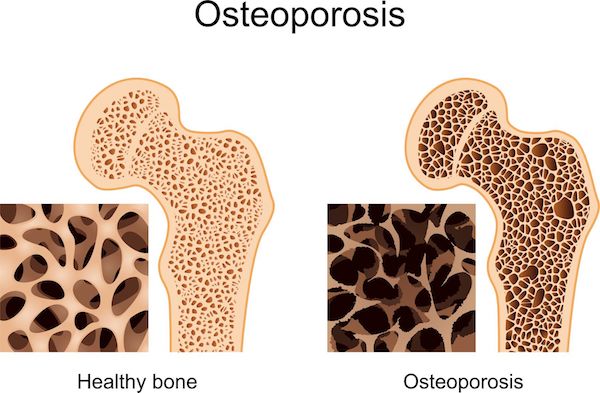
It occurs when bone is broken down faster than it can regenerate, which tends to happen as we age. Women are particularly at risk of developing osteoporosis as they tend to have smaller frames, which means less total bone mass. There is also a link between osteoporosis and menopause, as the reduction in oestrogen levels is tied to a faster loss of bone mineral density. A family history of the disease also puts you at greater risk of developing it yourself.
The bone disease may be secondary to other medical conditions, including underactive gonads, overactive adrenal glands or thyroid gland, and vitamin deficiencies. It’s also associated with rheumatoid arthritis, alcoholism, diabetes, epilepsy and chronic lung disease.
What are its symptoms?
According to the National Osteoporosis Foundation South Africa, osteoporosis ‘symptoms’ are rare, with the first real sign of the disease often being a broken bone, making it a dangerous but silent disease. In some cases, loss of height may occur as a result of multiple fractures to the vertebrae of the spine.
How is it diagnosed?
There are several tests that can be ordered by your doctor in order to reach an osteoporosis diagnosis. The National Osteoporosis Foundation says that these include various X-rays to measure bone density, such as the DXA scan (dual X-ray absorptiometry), which is considered the gold standard test for the disease, and QCT (ultrasound and quantitative computed tomography). Usually these diagnostic X-rays will only test a few bones, most commonly the wrist, hip and spine.
Then there are also blood tests which look for certain markers in the blood.
What are your treatment options?
Osteoporosis treatment may depend on the extent of the bone density loss. In some cases, lifestyle changes may be all that is needed, while in others osteoporosis drugs called bisphosphonates may be used to inhibit the cells that break down bone, or hormone-related therapies may be used.
The most important lifestyle modifications are quitting smoking and reducing alcohol intake, as both habits have been linked to reduced bone density. This includes regular load-bearing exercise too, as this has been shown to help maintain and even increase bone density, and eating a healthy diet rich in bone-building calcium and vitamin D.
Can it be prevented?
While certain osteoporosis risk factors are non-modifiable (gender, age, genetics, etc.), making a choice not to lead a sedentary lifestyle, smoke or drink more than two units of alcohol per day can slow the rate at which you lose bone density.
The correct diet is also essential for osteoporosis prevention – be sure to include at least 1 000mg of calcium per day (1 200mg for women over 50 and men over 70) and vitamin D to help your body absorb the calcium. Good sources of calcium include dairy products, sardines, soy products, dark green leafy vegetables and fortified cereals.
For more info
The National Osteoporosis Foundation
IMAGE CREDIT: 123rf.com
