Sickle cell anaemia – also known as homozygous haemoglobin S or S-thalassaemia – is an inherited blood disorder that affects the haemoglobin (a protein that carries oxygen) in the red blood cells.
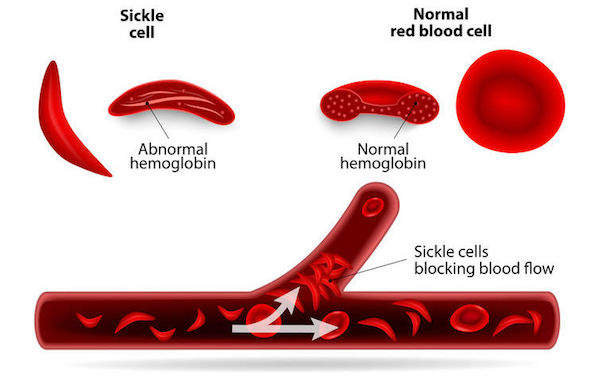
Healthy red blood cells are round and flexible enabling them to move easily through small blood vessels to do their work of delivering oxygen. With sickle cell disease, the red blood cells become a crescent or sickle shape. These blood cells die off faster than healthy cells, break apart easily, and tend to clump together in blood vessels blocking flood flow.
This can result in severe pain (known as sickle cell crisis – a medical emergency), and permanent damage to the brain, heart, lungs, kidneys and liver. The absence of healthy red blood cells to carry adequate oxygen to all parts of the body results in anaemia.
Its causes lie in a genetic abnormality in the haemoglobin gene. It will affect children born to parents who both have sickle haemoglobin genes.
What are its symptoms?
Sickle cell anaemia symptoms include the following:
- Anaemia
- Fatigue
- Swollen hands and feet (referred to as hand-foot syndrome)
- Episodes of pain in the chest, abdomen and joints (caused when the sickle cells block blood flow through small blood vessels)
- Frequent infections
- Delayed growthâ¨
- Vision problemsâ¨
- Fever
- Paleness in the skinâ¨
- Paralysis or weakness (possibly indicating a stroke)
How is it diagnosed?
Sickle cell anaemia is usually diagnosed during infancy. Diagnosis can be confirmed with a blood test called a haemoglobin electrophoresis, which can measure the amount of abnormal haemoglobin. It can determine whether the individual is a carrier (known as sickle cell trait) or if they have sickle cell disease.
Prenatal testing by examining DNA in foetal cells obtained during an amniocentesis (a prenatal test where a small amount of amniotic fluid is removed from the sac surrounding the foetus for testing) can also be performed. Early detection and treatment reduces the risk of serious infections and complications.
Genetic counselling may be recommended if you or your child is tested positive for sickle cell trait or sickle cell anaemia.
What are your treatment options?
Treatment involves managing the symptoms, and includes:
- Opioid pain medication (for example, morphine)
- Anti-inflammatory medication (for example, ibuprofen)
- Antibiotics for infection
- Oxygen supplementation
- Blood transfusion
A medication called hydroxyurea has been used to prevent painful episodes of sickle cell disease. Regular use decreases the frequency and severity of sickle cell crisis.
The only curative measure is a stem cell transplant from a matching donor. When successful, the transplants have resulted in patients being cured, with no further episodes of pain. It is, however, a risky procedure with a 5 to 10% mortality rate.
Current research is aimed at preventing the sickling of red blood cells and improving blood flow and delivery of oxygen, with treatment trials currently underway.
In children diagnosed with sickle cell syndrome, vaccinations to prevent infections are recommended.
Can it be prevented?
Sickle cell anaemia is an inherited condition. Genetic counselling is recommended if one or both parents have the sickle cell trait. Once diagnosed, certain measures can be taken to help avoid complications, including:
- Taking folic acid supplements and following a healthy dietâ¨
- Keeping hydrated; dehydration can precipitate sickle cell crisis
- Avoiding extreme heat or cold
- Discussing an exercise plan with your doctor
- Being aware of side-effects of over-the-counter medication, as certain meds can constrict the blood vessels
- When planning a trip to a high altitude area, discuss oxygen supplementation with your doctor.
IMAGE CREDIT: 123rf.com
