Glomerulonephritis – also known as nephritis – is a potentially life-threatening kidney disease that can lead to kidney failure.
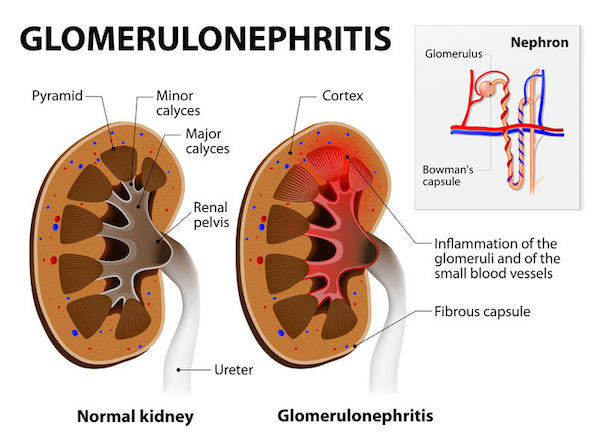
Glomeruli are structures in your kidneys that are comprised of tiny blood vessels and tubules. They help filter your blood and remove excess fluids, electrolytes and waste from your urine, passing them into your urine.
If they are damaged by glomerulonephritis (GN), which causes them to inflame, your kidneys stop working properly and lose their filtering ability, resulting in the build-up of dangerous levels of fluid, electrolytes and waste.
You could develop nephrotic syndrome (also known as nephrosis), which severely depletes the protein in your urine, leading to fluid and salt retention, and ultimately high blood pressure (hypertension), high cholesterol and swelling throughout your body (oedema). If this isn’t brought under control, kidney (renal) failure could occur.
GN can also lead to the following fallout:
- Acute kidney failure
- Chronic kidney disease
- Recurrent urinary tract infections (UTIs)
- Congestive heart failure
- Electrolyte imbalances, for example, high levels of potassium or sodium
- Malignant high blood pressure
- Pulmonary oedema
Primary glomerulonephritis is when GN occurs on its own, while secondary GN is when another disease such as lupus or diabetes is its cause. GN can be acute (sudden) or chronic (long-term or recurring).
The following conditions may cause GN:
- Abuse of non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen
- A genetic disease such as hereditary nephritis
- Amyloidosis (where abnormal proteins damage organs and tissues)
- Bacterial endocarditis (infection of your heart valves)
- Diabetes
- Exposure to hydrocarbon solvents
- History of certain cancers, for example, ovarian or pancreatic cancer
- Immune diseases such as Goodpasture’s syndrome (a rare autoimmune disease which impacts your kidneys and lungs) and lupus (systemic lupus erythematosus, or SLE)
- Polyarteritis nodosa (a disease of the arteries)
- Strep throat infection
- Viral infections including HIV/AIDS, hepatitis B and C
- Wegener’s granulomatosis (a rare disease of the arteries)
However, in many cases, the exact cause is unknown.
It’s pronounced gloe-mer-u-low-nuh-FRY-tis.
What are its symptoms?
The symptoms and signs of acute GN include:
- Blood in your urine
- Fluid in your lungs, causing coughing
- High blood pressure (hypertension)
- Puffiness of the face (oedema)
- Shortness of breath
- Urinating less than usual
As mentioned already, chronic GN can develop with no symptoms, although symptoms similar to acute GN may develop gradually. Other symptoms could include:
- Abdominal pain
- Bubbly or foamy urine
- Frequent night-time urination
- Frequent nose bleeds
If GN has progressed to an advanced stage, you could display the following symptoms of kidney failure:
How is it diagnosed?
Your doctor will do a physical examination checking your signs and symptoms, and speak to you about your medical history. This will be followed by a urine test (urinalysis) to check for blood and protein in your urine, which are important markers of the disease, and blood tests.
These tests may also be needed to confirm a diagnosis:
- A biopsy of your kidneys (a small sample of one of your kidney’s tissue taken with a needle)
- Chest X-ray
- CT (computerised tomography) scan
- Kidney ultrasound
- Immunology tests
- X-ray of kidneys with dye (intravenous pyelogram)
What are your treatment options?
The treatment of glomerulonephritis depends on its type. If you have acute GN and it is caught early enough, it can be temporary and reversible. Chronic GN may also be slowed with early treatment. The goal of treatment is always to protect your kidneys from further damage.
One of the main treatments is to ensure your high blood pressure (hypertension) is brought under control. Your doctor may do this by prescribing medications such as angiotensin-converting enzyme inhibitors (ACE inhibitors) and angiotensin II receptor blockers (ARBs).
If your kidneys are being damaged by your immune system, corticosteroids will be prescribed to reduce immune response. A special blood filtering procedure called plasmapheresis that removes harmful proteins may be recommended.
When it comes to chronic GN, your diet will need to be overhauled with the help of a dietitian so that the amount of protein, salt and potassium in your diet is decreased substantially. You may be prescribed diuretics (water pills) to reduce swelling, and calcium supplements.
If you develop kidney failure, you may need dialysis (an artificial kidney machine that filters your blood) and you may even need a kidney transplant.
Can it be prevented?
There is unfortunately no way to prevent most cases of glomerulonephritis, although some cases may be prevented by limiting exposure to hydrocarbon solvents and nonsteroidal anti-inflammatory drugs (NSAIDs).
Also, practising safe sex and avoiding illicit intravenous (IV) drug taking so that you don’t become infected with HIV/AIDS or hepatitis will aid prevention.
To both recover from glomerulonephritis and prevent developing it again, you should take these crucial preventative steps:- Control your blood sugar level if you have diabetes
- Control high blood pressure (hypertension)
- Maintain a healthy weight
- Quit smoking
- Restrict potassium, protein and salt in your diet
- Seek prompt medical assistance if you develop a strep throat infection
IMAGE CREDIT: 123rf.com
