Hashimoto’s thyroiditis, also known as autoimmune thyroiditis or lymphocytic thyroiditis, is a common autoimmune disease in which the thyroid gland comes under attack by the body’s own immune system.
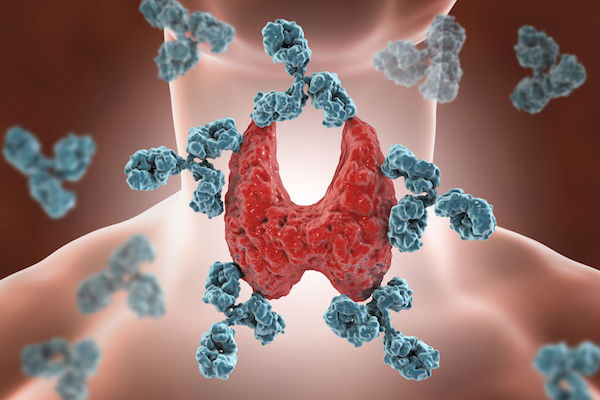
Hashimoto’s thyroiditis is a condition characterised by damage to the thyroid gland in the front of the throat inflicted by antibodies created by the body’s own immune system, ultimately leading to hypothyroidism, also known as an underactive thyroid, which sees too little thyroid hormone being produced.
The causes of Hashimoto’s thyroiditis are not largely understood, but some research indicates there may be a genetic factor as it frequently runs in families.
Other risk factors for the development of Hashimoto’s thyroiditis include excessive iodine intake in those who may have a genetic predisposition for thyroid disease, other pre-existing autoimmune disorders, being female (it occurs in an estimated seven times as many women as men) and radiation exposure.
What are its symptoms?
Hashimoto’s thyroiditis symptoms develop slowly, with the disease sometimes progressing over years before showing obvious signs.
Those with Hashimoto’s thyroiditis may suffer from:
- Fatigue
- Weight gain
- Pallor and puffiness of the face
- Hoarseness
- Swelling of the thyroid gland in the front of the throat (called a goitre)
- Frequently feeling cold
- Constipation
- Difficulty conceiving or carrying a pregnancy to term
- Dry skin, brittle hair and hair loss
- Pain in the joints and muscles
- Irregular or heavy periods
- Depression
- Panic disorders
- Slow heart rate
Untreated Hashimoto’s thyroiditis can lead to myxedema coma, a life-threatening complication of a severely underactive thyroid (hypothyroidism). This is why it’s essential to always have the above symptoms evaluated by a doctor.
How is it diagnosed?
Once all your signs and symptoms have been assessed, there are various tests that may be used to confirm a Hashimoto’s thyroiditis diagnosis. A blood test to determine the level of thyroid stimulating hormone (TSH) in your system is one useful indicator – TSH levels are high in those with Hashimoto’s thyroiditis as a result of the pituitary gland attempting to compensate for the thyroid’s sluggishness by providing more of the chemical that stimulates it to work.
Blood tests can also pick up the specific anti-thyroid antibodies created by the immune system to attack the thyroid as a result of this condition.
What are your treatment options?
There is no cure for Hashimoto’s thyroiditis as yet but the condition can be effectively managed with thyroid hormone replacement medications. Treatment for Hashimoto’s thyroiditis – usually a daily pill – will need to be taken life-long, but when used as prescribed, all symptoms of an underactive thyroid (hypothyroidism) should be alleviated.
There has been some evidence to suggest that using a selenium supplement may slow the progression of the disease, but further clinical trials are needed to support this claim. Boost selenium in your diet with Brazil nuts, tuna and wholewheat bread – all rich sources of this trace element.
Can it be prevented?
As much remains to be understood about the development of Hashimoto’s thyroiditis and why some people’s immune systems malfunction in this way, there is no sure way to prevent it.
Factors such as high iodine intake and a deficiency of the dietary mineral, selenium, have been identified as possibly contributing to autoimmune thyroid disease in genetically at-risk individuals, so if Hashimoto’s thyroiditis runs in your family it may be worth consulting your doctor on how to lower your risk.
IMAGE CREDIT: 123rf.com
